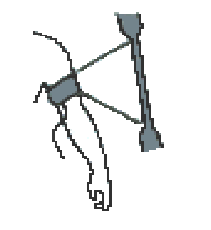Curriculum for the DynaPulse 200M Complete Educational System
Table of Contents
Introduction
The DynaPulse 200M, Education Edition, a microcomputer based
lab (MBL), combines curriculum and medical instrumentation with interactive,
easy-to-use software to demonstrate the practical applications of computer
and medical technologies. Educators have access to a modern educational method
to teach cardiovascular function that is designed for students to identify
the biological, anatomical, physiological, and physical education applications.
The curriculum begins with simple definitions of blood pressure
and hypertension and goes on to describe the techniques for blood pressure
determination and the cardiovascular system in more depth. Also included are
five labs designed to provide practical hands-on approach to cardiovascular
monitoring.
DynaPulse is used in many physicians’ offices, hospitals,
medical universities, and research facilities across the U.S. and worldwide.
Students may explore cardiovascular function in their future work with the
same DynaPulse available for the classroom today.
Blood Pressure and Hypertension
One of the most important determinants of cardiovascular function
is the blood pressure. The blood pressure is defined as the force or pressure
of the blood against the vessel walls of the cardiovascular system. Blood
pressure is transient and fluctuates as a result of the pulse cycle. When
the heart contracts, pushing blood out of the heart and into the vessels of
the cardiovascular system, the blood pressure increases, and the maximum pressure
in the vessel is known as the systolic blood pressure (SBP). In contrast,
when the heart relaxes in between heart beats (pulses), the pressure in the
vessels decreases and the lowest pressure is referred to as the diastolic
blood pressure (DBP). Clinically, the systolic and diastolic blood pressures
are denoted as the systolic pressure over the diastolic pressure. For example,
a systolic pressure of 120 mmHg and diastolic pressure of 80 mmHg, would be
referred to as “120 over 80”. Although pressure can be recorded
in several different units, clinically, blood pressures are measured in millimeters
of mercury (mmHg).
The systolic and diastolic pressures are two of several independent
values representing the cardiovascular performance of the heart. Clinically,
these two values can be combined to form an average blood pressure, called
the mean arterial pressure, which reflects the influence of the systolic and
diastolic pressure on the cardiovascular system. The mean arterial pressure
(MAP) is the time weighted average of the blood pressure during the entire
pulse cycle. During a single pulse, approximately one third of the cycle is
maintained near the systolic pressure, and two thirds of the cycle is maintained
near diastolic pressure. Therefore, estimated:
MAP = 1/3 SBP + 2/3 DBP
The calculation of the main
arterial pressure is an excellent way to evaluate the stress on
the walls of the vessels. This new parameter may be useful to
quickly evaluate excessive load on the cardiovascular system in
the future.
Hypertension:
Blood pressure not only fluctuates due to the pulse cycle,
but also as a result of external factors. Diet, stress, and physical exertion
are only a few of the factors that may influence blood pressure changes. However,
in healthy individuals, the blood pressure will return to “normal”
when external factors are minimized or negligible. In contrast, when the blood
pressure remains high for an extended period of time, an individual may be
diagnosed as having high blood pressure/hypertension. Hypertension is a serious
disorder that affects approximately 50 million American adults. Hypertension
is not necessarily difficult to treat, however, it is hard to detect because
it shows no symptoms and therefore is known as the “silent killer.”
Some people claim that they can feel high blood pressure, but estimates are
rather unreliable. Only by performing regular measurements with an accurate
method can one assess the blood pressure and cardiovascular health.
In recent years, medical research has revealed a link between
hypertension and other cardiovascular diseases. The elevated blood pressure
resulting from hypertension, can cause excessive stress on the heart and blood
vessels. As a result of the excessive load, the risk of heart attack and stroke
increases substantially. In order to help prevent cardiovascular disease,
early detection of hypertension is critical. The National Institute of Health
(NIH) has developed guidelines (1997) in order to assess blood pressure status.
The guidelines have been developed to more clearly define hypertension as
a cardiovascular risk factor and provide direction for intervention.
The blood pressure classifications, defined by the NIH, are
based on the average of at least two blood pressure measurements for an adult,
assuming they are not on anti hypertension medication nor actually ill.
| Category
|
Systolic
(mm Hg) |
Diastolic
(mm Hg) |
| Optimal |
<120 |
<80 |
| Normal |
<130 |
<85 |
| High Normal |
130-139 |
85-89 |
| Hypertension: |
|
|
| stage 1 |
140-159 |
90-99 |
| stage 2 |
160-179 |
100-109 |
| stage 3 |
> or equal
180 |
> or equal to
110 |
When the systolic and diastolic blood pressures fall into different
categories, the higher category should be selected to classify the blood pressure
status. For example, 160/92 should be classified as “moderate” and
180/92 should be classified as “very severe.” In addition, a classification
of Isolated Systolic Hypertension (ISH) may be made when SBP>140 and DBP<90.
Therefore, a blood pressure of 160/82 Should be classified as "ISH".
Once a blood pressure classification has been established,
the following guidelines should be used as a reference for follow-up.
| Initial Screening Blood
Pressure (mmHg) |
Initial Screening Blood
Pressure (mmHg) |
|
| Systolic |
Diastolic |
Followup Recommended |
| <130 |
<85 |
Recheck in 2 years |
| |
85-89 |
Recheck in 1 year |
| |
|
Confirm within 2 months |
| |
|
Evaluate or refer to source of care within 1 month |
| |
|
Evaluate or refer to source of care immediately, or within 1 week depending on clinical situation. |
If the systolic and diastolic blood pressure fall into different
categories, follow the recommendations for the shorter follow-up.
By regularly calculating the blood pressure and following the
structure guidelines developed by the NIH, one can reduce hypertension and the
risk of cardiovascular disease.
Cardiovascular Physiology
Structures of the Heart:
The heart serves as the central pump for the cardiovascular
system and is responsible for moving the blood to the tissues of the
body. About the size of a person’s fist, and composed of four separate
chambers, the unique size and structure of the heart (figure 1) is truly
remarkable, providing an excellent adaptation of mechanics. The chambers
are broken down into the left and right atria, which are small chambers
in the upper heart, and the left and right ventricles, the strong powerful
chambers in the lower heart. The muscular wall of the heart, or the
myocardium, is subdivided into four distinct muscle layers overlapping
and wrapping around the heart to produce a wringing motion that is responsible
for the pumping action. The myocardium is primarily composed of cardiac
muscle fibers that resemble skeletal muscle due to striations or stripes
across the fiber. The myocardium is lined with an inner layer of endocardium
and covered with an outer layer called the epicardium. The entire package
is situated in a fibrous sac, the pericardium, containing a small quantity
of pericardial fluid that helps reduce friction between the heart and
other organs.
Several other structures of the heart are important
in the establishment of the blood flow direction through the heart.
The intra-atrial septum divides the left and right atria and the intraventricular
septum divide the ventricles, creating a double pump system within the
same organ. Thus, it is sometimes convenient to refer to the left and
right heart as if they were separate units although both sides of the
heart act simultaneously in a heartbeat. The atrioventricular (AV) valves
are sheets of connective tissue employed to separate the atria from
the ventricles. The right AV valve is made up of three cusps or leaflets
called the tricuspid valve. The left AV valve has two leaflets, thus
called the bicuspid valve, and also known as the mitral valve. These
AV valves allow ventricular filling of blood, while simultaneously preventing
the back-flow of blood back into the atria during ventricular contractions.
Two other valves (semilunar valves), situated at the beginning of the
pulmonary artery and aorta, avert back-flow of the blood to the heart
from the pulmonary and systemic circulation.
|
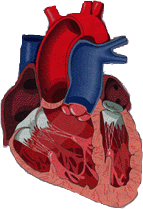
Figure 1
|
Electrical Conduction:
The pattern of conduction for contraction of the heart is
an electrical coupling event between cardiac muscle cells. Cardiac cells can
be divided into three functional classes: myocardial or contractile cells,
pacemakers or nodal cells, and conducting cells. The myocardial cells make
up about 99% of the heart’s mass and are responsible for contraction
and force generation. The second class of cells, pacemaker cells, provide
the rhythmic electrical signals that will spread across the whole heart, causing
a wave of contractions (heartbeats). Pacemaker cells can be found at the sinoatrial
(SA) node and the atrioventricular (AV) node of the heart. The SA node has
the highest rate of rhythmic discharge and is considered the heart’s
natural pacemaker.This cluster of pacemaker cells determines the frequency
of heartbeats, or heart rate. The signal that initiates in the SA node travels
to the AV node where it is delayed. The third class of cells, conducting cells,
form a conduction system specialized for conducting a signal rapidly from
one part of the heart to another. From the AV node the signal follows a tight
network of conducting cells known as the bundle of His. The bundle of His
is comprised of one right, and two, left bundle branches that direct the signal
to the lower tip (apex) of the heart. These branches curve back up to form
a complex network of Purkinje fibers beneath the endocardium of the two ventricles,
causing synchronized contraction throughout the heart.
Circulatory System:
The circulatory system is composed of the heart and an intricate
system of vessels responsible for delivering blood to the tissues of the body
and back to the heart. Three types of vessels complete the task of blood delivery.
They are arteries; elastic blood vessels that carry blood away from the heart,
capillaries; the smallest vessels in the body and the major site for exchange
of materials between blood and tissues, and veins: vessels that carry blood
back to the heart.
The circulatory system is arranged as a circuit composed of
two major loops. The first loop is known as the systemic circulation. Blood
leaves the left ventricle through the aorta and is delivered to the tissues
of the body before returning to the right atrium through the vena cava. In
the systemic capillaries, the blood gives up some of its oxygen in exchange
for carbon dioxide, produced by tissue metabolism. The pulmonary circulation
comprises the second loop of the circuit and primarily found on gas exchange.
Blood leaves the right ventricle through the pulmonary artery and is delivered
to the lungs for gas exchange. The pulmonary vein returns blood to the left
atrium from the lungs. In the pulmonary capillaries, the burden of carbon
dioxide acquired by the blood in the systemic capillaries is transferred to
pulmonary gas, and the oxygen that was unloaded in the systemic loop is replaced.
Another important system is the coronary circulation, which
is actually a component of the systemic circulation. The coronary arteries
branch from the beginning of the systemic circulation and serve the capillaries
of the heart itself. Venous blood is returned to the heart by the coronary
sinus. Maintenance of the heart tissue is possible by the coronary circulation.
Blood Components:
Blood consists of three types of cells suspended in a liquid
called plasma. The three types are red blood cells (RBC), white blood cells
(WBC), and platelets. The red blood cells form the largest percentage of blood
cells and are primarily devoted to the transport of nutrients to the body.
Red blood cells, also known as erythrocytes, set aside 25% of their cytoplasmic
volume for an iron containing protein, hemoglobin, responsible for oxygen
transport and update of carbon dioxide wastes from the living tissues. Clinically,
the amount of red blood cells is known as the hematocrit. The hematocrit is
the percentage of total blood volume composed of red blood cells. Normal hematocrit
volume for men varies between 40%-50% and for women ranges between 35% - 45%.
Unlike red blood cells, white blood cells are divided into
two groups, the granulocytes whose primary purpose is to engulf and digest
bacteria and other foreign materials, and non-granulocytes, which are responsible
for specific immune response in the body. The platelets make up the last type
of blood cell. Platelets play a critical role in the formation of clots, which
reduce blood loss following injury.
Simple Fluid Mechanics
Pipe Mechanics:
To understand blood flow in the cardiovascular system, one
must understand simple fluid mechanics. Pressure, flow, and resistance are
all fundamental elements of fluid mechanics. The relationship between these
parameters clearly defines the behavior of the blood in the heart and vessels
of the human body. The fundamental equation of fluid mechanics is a derivative
of Ohm’s Law. Simply stated:
Pressure = Flow x Resistance
Pressure is measured in
millimeters of mercury (mmHg), flow is measures in liters per
minute (L/min), and resistance is measured in millimeters of
mercury per liter per minute (mmHg/L/min).
Artery Mechanics:
In order to understand blood flow at the local level, one
must examine a single straight arterial segment. Therefore, the fundamental
equation becomes:
Mean Arterial Pressure = Arterial flow x Peripheral Resistance
The local equation considers only
the flow of blood through a single arterial segment. The arterial
flow is the volume of blood flowing through the segment per
minute which is dependent on both the cross sectional area of the
arterial segment (a) and the velocity (u).
Arterial flow = cross sectional area (a) x velocity (u)
Therefore, as an example, a large
artery with a slow flow velocity or a small artery with rapid
flow velocity can maintain the same flow rate.
The peripheral resistance is the
resistance of the artery to the flow and it is dependent on both
the cross sectional area (a) and the elasticity (ke) of the
arterial segment.
Peripheral Resistence = 1/a x 1/kehard
For example, if an artery is hard
and thin it will provide great resistance to blood flow.
Cardiovascular Mechanics:
In contrast, in order to evaluate the behavior of the complete
cardiovascular system one must examine the heart and all the vessels of the
body. Therefore, our fundamental equation becomes:
Mean Arterial Pressure = Cardiac Output x Systemic Vascular Resistance
The cardiovascular system equation
takes into account not just a single artery, but the entire
vascular system. In this case, the cardiac output reflects the
volume of blood exiting the heart and entering the arterial
system per minute. The cardiac output is dependent on both the
stroke volume (SV), which is the volume of blood ejected per
contraction, and the heart rate (HR).
Cardiac Output = Stroke Volume (SV) x Heart Rate (HR)
The systemic vascular resistance
is the resistance of the vasculature to the flow. Much like the
peripheral resistance, the systemic vascular resistance is
dependent on the cross sectional area. However, in this case it
is dependent on the total arterial cross sectional (A). In
addition, the elasticity of the entire arterial system (KE) must
be evaluated.
Systemic Vascular Resistance =1/A x 1/Ke
Height Dependent Pressure Variations:
A fundamental property of pressure is that the pressure is
the same for all points at a certain level. For example, the pressure at the
surface of a pool is the same for all points. However, as the depth increases
the pressure also increases as a result of hydrostatic pressure. Hydrostatic
pressure is defined as the pressure due to a fluid. Therefore, the pressure
at depth is defined as:
PDepth = PSurface + p x g x h
In which P Depth is defined as the pressure
at a depth (h) below the surface, measured in millimeters of
mercury (mmHg), r is the density of the fluid which is defined as
mass of the fluid per volume, (Water = 1.0 kilograms/Liter), g is
the acceleration due to gravity (m/sec 2), and h is the depth
below the surface (meters).
Hydrostatic pressure not only applies to simple physical examples
but also to the human body. For example, the cardiovascular system must constantly
adjust to changes in pressure due to hydrostatic pressure. As one moves from
a sitting to standing position, the vessels of the legs must constrict to
counterbalance the additional pressure caused by an increase in height. A
similar reflex may occur in the arm as it is raised, however, in this case
the vessels relax to adjust to a decrease in height. In the first case, the
vessels of the legs constricted due to the increase in hydrostatic load, and
in the second case the vessels of the arm dilated due to the decrease in hydrostatic
load.
Cardiovascular Parameters
The behavior, health, and status of the cardiovascular system
can be described in many ways. One of the most popular techniques is to evaluate
certain cardiovascular parameters that may be used as an index to cardiovascular
fitness. They are as follows:
Heart Rate (HR): The number of beats (contractions) per minute. [beats/min]
Stroke Volume (SV): The stroke volume is the volume of blood ejected from
the heart during heart contraction. [ml]
Cardiac Output (CO): The cardiac output is the volume of blood ejected from
the heart per minute.
Cardiac output is calculated as: CO = SV X HR [L/min]
Peripheral Resistance (PR):
The peripheral resistance is the effect of the
vessels resisting flow. The peripheral resistance is primarily a function of
vessel size and of the number of vessels open. It can be calculated by the following:
PR = MAP/CO [mmHg/(L/min)]
Compliance (C):
The compliance is a relatively new cardiovascular
parameter that was developed to assess the elasticity or rigidity of the heart
and arteries. The compliance is calculated as:
Change in Volume/Change in Pressure
In order to assess the systemic
compliance, which is the compliance of the heart and large
arteries, the change in volume of the heart (stroke volume) is
divided by the change in pressure within the heart (systolic
pressure minus the diastolic pressure):
C = SV/(SBP-DBP) x [ml/mmHg]
Blood Pressure Regulations
Homeostasis:
Homeostasis is defined as the condition of constancy of the
“internal environment” in terms of its cells, tissues, and organs.
Thus in blood pressure regulation, homeostasis will tend to stabilize the
blood pressure, maintaining it at a steady resting state. For example, if
a person exercises, the heart rate will increase, inducing higher blood pressure.
Homeostasis will accommodate the body through various mechanisms to decrease
the heart rate and reduce the high blood pressure. Homeostasis is the primary
basis by which normal body functions are maintained in order to sustain life.
Negative Feedback System:
One of the most important techniques for maintaining homeostasis
is the negative feedback system. The system works to maintain a physiological
set-point of the body by sensing changes and returning the body to the original
set-point. That means, if a physiological disturbance occurs, the body via
a negative feedback system will counteract the disturbance and try to return
the body to its normal set-point. There might be more than one negative feedback
systems that can counter the changes of a particular disturbance (as is the
case of blood pressure regulation). Whenever the condition of constancy is
deviated and corrections are not possible, damage to the body and death can
result.
Some of the important tools to
regulate blood pressure in the body are as follows:
Baroreceptors:
Baroreceptors are pressure sensors which monitor blood pressure.
One population of these receptors is located in the walls of the common carotid
artery, forming the carotid sinus. Others are scattered throughout the wall
of the aortic arch. They are very sensitive to blood pressure leaving the
heart and act as the sensor to keep the overall pressure of the heart at a
set point. If the blood pressure begins to fall, baroreceptors activation
decreases, and the autonomic nervous system acts to increase blood pressure.
In contrast, if the blood pressure increases, baroreceptor activation also
increases, and the autonomic nervous system must act to decrease the blood
pressure.
Vasodilation:
Smooth muscles of most vessels are innervated by the autonomic
nervous system. When blood vessels “dilate” or vasodilate through
relaxation of the smooth muscles in the wall of the vessels, the radius and
compliance of the vessels increase. Not only does the larger opening in the
vessels increase blood flow through the vessels, but also the larger compliance
gives the vessels the ability to stretch with an increased load, permitting
an even greater volume of blood flow through the vessels.
Vasoconstriction:
Similar to vasodilation, vasoconstriction is also controlled
by the autonomic nervous system, and causes the smooth muscles in the wall
of the blood vessel to “constrict” or vasoconstrict. As a result
of vasoconstriction, the vessels stiffen and become less compliant. However,
the effects of vasoconstriction in the arteries and veins are quite different.
In arterial vasoconstriction (major site of flow resistance in the body),
the effect is to redirect blood flow and increase the total peripheral resistance.
In the veins, vasoconstriction does not affect total peripheral resistance
as greatly as in the arteries, which have lower overall compliance (stiffer).
Instead, the primary outcome of vasoconstriction is to decrease the venial
wall compliance, which decreases the volume of blood within the veins.
Precapillary Sphincters:
Located at the entrance to the capillary vessels are precapillary
sphincters consisting of a single smooth muscle fiber per sphincter. These
capillary “gate- keepers” open and close in response to changes
in their immediate environment, such as blood pressure. This helps to maintain
blood pressure in the venous circulation. Another important function of the
precapil lary sphincter is to prevent back flow of blood, driving blood flow
in one direction.
History of Blood Pressure Measurement
In 1733, Reverend Stephen Hales published one of the first
methods of blood pressure measurement. He developed a technique in which a
glass tube could be inserted into the arteries of the neck of a horse. By
holding the glass tube in an upright position, the blood would be pumped out
of the neck and into the tube by the pumping of the heart. As a result, the
level of the blood in the tube could determine the blood pressure. Unfortunately
for the horse, since the blood in the tube was not returned to the cardiovascular
system, the measurement was irreversible.
The tools for the direct assessment of blood pressure have
come a long way since the early 1700’s. Today, direct techniques of blood
pressure evaluation called catheterization take place in hospitals around
the world daily. Catheterization involves inserting a pressure transducer
known as the catheter, into different areas of the cardiovascular system.
For instance, in order to understand the pressure changes inside the left
ventricle of the heart, the catheter is inserted into the femoral artery of
the patient (the groin area), guided up the femoral artery into the aorta,
past the aortic valve and into the left ventricle. The results of the catheter
pressure are displayed as a waveform on the screen of a computer system. Although
discomforting, in most cases the patient experiences no long-term side effects.
Catheterization procedures, however, have several drawbacks.
First, the procedures can only be performed in a sterile environment such
as a hospital under the supervision of a cardiologist. Second, due to the
need for infection control and professional personnel, most catheterization
procedures are time consuming and extremely expensive ranging in the thousands
of dollars. Finally, as a result of any invasive procedure, the patient is
under the risk of complications such as infection, which may lead to very
serious consequences. As a result of these weaknesses, great time and effort
was taken in the development of new fast and convenient methods of blood pressure
measurement. The development of indirect blood pressure measurement techniques
has reduced cost, time and risk of complications to the patient making indirect
blood pressure assessment the standard technique for regular blood pressure
evaluation.
Non-Invasive Blood Pressure Measurement Techniques
During the past 90 years two primary methods of non-invasive
blood pressure assessment have been developed. Although they depend
on different mediums in order to detect the blood pressure signal, both
the auscultatory and oscillometric techniques depend on the use of an
air filled cuff to occlude the brachial artery. Cuff measurement principles are based on simple fundamental physics.
As illustrated in Figure 2, when the cuff is inflated to a pressure
greater than the maximum arterial pressure (systolic pressure), no blood
flows through the artery under the cuff. When the cuff slowly deflates
to a pressure equal to the systolic pressure, blood begins to flow through
the artery (figure 3). As the cuff pressure continues to deflate, the
oscillation of blood jetting through the artery begins to flow stronger.
When the cuff no longer occludes the artery and the artery has returned
to the original state (figure 4), the minimum pressure (diastolic pressure)
is observed. Both indirect methods of assessment depend on this simple
physical phenomenon.
The auscultatory method of blood pressure determination
depends on sound to transmit the blood pressure signal. The physical
phenomenon due to the cuff occluding the brachial artery is detected
by the human ear through a stethoscope. The Korotkoff sound signals,
as they are known, correlate to characteristics of the cuff deflation
principle.As the pressure decreases from above
the systolic pressure due to the deflation of the cuff, the Korotkoff
sounds become audible and then fade away as the cuff pressure decreases.
The systolic pressure is the pressure at which the Korotkoff sounds
first become audible. The sounds then become muffled as the blood jets
through the brachial artery and finally disappear.The
pressure at which the sounds become extremely muffled and disappear
is the diastolic pressure. Unfortunately, inaccurate blood pressure
determination may occur due to hearing problems or noisy backgrounds,
in addition to inherent limitations of the human ear. However, an automated
auscultatory technique using a microphone may improve inherent limitations
of the manual technique providing more accurate blood pressure determinations.
|
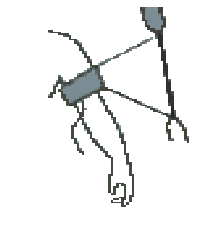
Figure 2
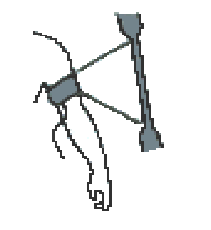
Figure 3
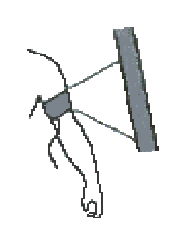
Figure 4
|
The oscillometric method of blood
pressure determination is dependent on pressure changes in the
brachial artery as air released from a pressure cuff. The
pressure volume coupling between the brachial artery and the cuff
is fundamental in the determination of blood pressure. A change
in blood pressure within the artery causes a change in volume of
the brachial artery due to the elasticity of the vessel. The
change in volume of the artery causes a change in volume in the
cuff due to the coupling of the cuff to the arm. A sensitive
pressure transducer that creates a digital signal detects the
corresponding pressure change within the cuff. The signal is
displayed as a blood pressure waveform (figure 5) in which blood
pressure can be calculated. The waveform is recorded as the cuff
pressure deflates from a cuff pressure greater than the systolic
pressure to cuff pressure that is less than the diastolic
pressure. Although traditional oscillometric methods use the
amplitude of the signal to detect the blood pressure, the
DynaPulse utilizes pattern recognition. Based on this technique,
a new patented algorithm is used to determine the systolic,
diastolic, and mean arterial pressure from the non-invasive blood
pressure waveform. The single pulse pressure wave (figure 6),
which is normalized to the systolic and diastolic pressures, is
utilized to examine individual pulse behaviors.
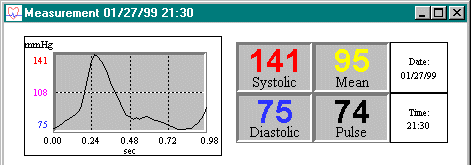
Figure 6: Single pulse waveform
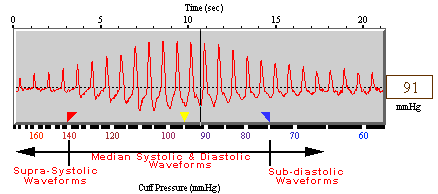
Figure 5: Three sections of
DynaPulse pressure waveforms
Pathology
In order to develop a broader
understanding of the cardiovascular system, it is important to
develop an understanding of cardiovascular complications and some
of the risk features that lead to heart disease.
Atherosclerosis:
A disease process that results in
the formation of abnormally thickened vascular walls due to
plaque. Plaque is characterized by the abnormal proliferation of
modified smooth muscle cells and large deposits of cholesterol.
When plaque formation develops and narrows the arteries,
especially in the heart and the brain, damage can result as a
reflection of blood deprivation. Also, plaque is considered to be
a foreign surface to the body, and clot formation can occur.
Therefore, if a clot develops in the coronary circulation,
preventing blood flow to the heart, myocardial infraction may
result. On the other hand, a stroke may occur from a blood clot
becoming dislodged in the brain. About 50% of all deaths from
heart disease in developed nations are the results of
atherosclerosis in the arteries of the heart and brain.
Coronary Artery Disease (CAD):
An umbrella term used for various
diseases that reduce or halt blood flow in the coronary arteries.
In most cases, atherosclerosis of the coronary artery reduces
blood flow to the heart over a period of years. Typically, the
patient receives a warning - chest discomfort known as Angina.
Angina indicates that a portion of the heart muscle is being
deprived of oxygen. If untreated, CAD may continue to cause chest
discomfort and result in a myocardial infarction or heart
failure.
Myocardial Infarction (MI):
A heart attack brought about by an
acute damage to the myocardium due to a sudden occlusion of the
coronary blood flow (lack of oxygen).
Heart failure:
A decrease in myocardial
contractility brought on by disease or damage. Heart failure may
be the result of a slow reduction in coronary blood flow over a
period of time, leading to progressive damage to the heart
muscle, or due to the accumulation of blood in the body, causing
excessive load on the heart.
Risk Factors and Prevention:
All of these cardiovascular
diseases are a function of many factors. Some of these factors
are uncontrollable, however, many factors can be minimized in
order to reduce the chance of a cardiovascular problem.
Uncontrollable Factors:
- Age (higher risk for elderly people)
- Sex (higher risk for men than women)
- Family history of heart attacks
Controllable Factors:
- High blood pressure (hypertension)
- High cholesterol level
- Smoking
- Lack of exercise
- Overweight
- Diabetes
- Alcohol
- Salty foods
- Constant work stress
- Personality (aggressive, self-confident, ambitious, persistent,
fast-paced, outgoing, and talkative)
By minimizing the impact of controllable factors, one can reduce the risk
of cardiovascular complications, and live a longer and higher quality life.
LAB 1: Ausculatory vs. Oscillometric Measurement Techniques
Suggested Time: 30 minutes
Purpose:
To compare two methods of indirect blood pressure measurement.
Materials:
- computer
- sphygmomanometer
- stethoscope
- DynaPulse hardware and software package
- paper and pencil
Procedure:
(You should work in
groups of 4 or 5)
Part A - Auscultatory Blood Pressure Measurement
1. The study group should be separated into sub-groups of two or three students
so that each member can take the blood pressure of another student.
2. Each subject should sit quietly for three minutes before completing a
measurement
3. Each student should take turns taking the blood pressure of another student
using the sphygmomanometer and stethoscope. (Auscultatory method)
4. The systolic and diastolic blood pressures should be recorded manually.
Part B - Oscillometric Blood Pressure Measurement
1. Each group member should sit quietly for three minutes prior to completing
a measure ment.
2. The oscillometric cuff should be placed on the arm of the subject and
the computer program activated to take a measurement.
3. In order to ensure an accurate measurement, the subject should relax
and minimize all movement including muscle contraction during the deflation
of the cuff.
4. Following the measurement, the oscillometric systolic blood pressure
(SBP) and dias- tolic blood pressure (DBP) should be compared to blood pressure
values obtained by the auscultatory method in part A.
5. In order to evaluate both methods for the accuracy of their mean arterial
pressure (MAP), it is necessary to estimate the MAP attained using the auscultatory
method by the following formula:
MAP = 1/3 SBP + 2/3 DBP
Compare the MAP calculations
derived by the auscultatory systolic and diastolic pressures with
the DynaPulse MAP.
LAB 2: Transient Blood Pressure Changes
Suggested Time: 50 minutes
Purpose:
To investigate the physiological changes in blood pressure as a result
of arm and body position, noxious stimuli, and mild exercise.
Materials:
- computer
- DynaPulse hardware and software
- container of ice water (0-2 degrees Celsius)
Note: In order to capture changes in blood pressure, the range
for blood pressure measurement may need to be changed. During the different
parts of the lab the systolic, diastolic, or both may either increase or decrease.
Procedure: (You will work in
groups of 4 or 5)
Part A - Rested Blood Pressure Changes
1. After each member has rested (sitting) quietly for three minutes, measure
each group member’s blood pressure using the DynaPulse oscillometric
system.
Part B - Arm Position Changes - The Gravity Effect
1. Have one subject rest in the seated position for three minutes.
2. Place the measurement cuff on the arm of the subject during the resting
stage.
3. Have one member of the group raise the relaxed arm of the subject above
the subject’s head while another member completes a measurement. For
best results make sure to hold the arm directly above the head and ensure
that the subject is not contract- ing the muscles of the arm.
4. Compare the subject’s base measurement from Part A with the results
of Step 3.
Part C - The Cold Reflex
1. Have a different member of the group rest in the seated position for
three minutes.
2. Have the measurement cuff placed on the arm of the subject.
3. Place the hand of the subject in a small bucket of ice water for approximately
two minutes. (Hand should be submerged to the wrist for the entire time
period).
4. After the two-minute period, remove the subject’s hand and place
arm at their side.
5. Complete another blood pressure measurement as soon as the arm is removed
from the ice water.
6. Compare the results of Part A with Step 5 for the subject.
Part D - Response to Exercise
1. Have a different member of the group jog in place for three minutes.
2. After three minutes, have the subject sit and immediately take a measurement.
3. Following two minutes of recovery, complete another measurement.
4. Compare the baseline measurement in Part A with both Steps 2 and 3.
Part E - Orthostatic Changes in Blood Pressure
1. Have one member of the group lay on a desk in a supine position for three
minutes.
2. After three minutes, take the subjects blood pressure using the DynaPulse.
3. Have the subject sit up, swinging their legs off of the table, and take
another mea surement. (Remember to minimize movement during the measurement)
4. Compare the results from Step 1 and 2 on your sheet.
LAB 3: Ergometer Training
Suggested time: 35 Minutes
Purpose:
To investigate the physiological changes in the cardiovascular
system as a result of exercis
Materials:
- cycle ergometer
- computer
- DynaPulse system hardware and software
Procedure:
During an eighteen-minute exercise study we will monitor several parameters
of cardiovascular function in order to achieve a better understanding of the
behavior of the body under physical stress. The subject will be required to
maintain a pedal rate of 80 rpm while the workload is incrementally increased
according to the schedule below. In order to achieve an accurate blood pressure
and heart rate reading it is essential that the subject discontinue all exercise
and remain still during each measurement stage. The DynaPulse is a clinical
grade oscillometric blood pressure monitor, and therefore any movement such
as minimal muscle contraction or repositioning of the arm will cause the pressure
signal to be distorted and skew the measurement. The arm should be held completely
still at the height of the heart by a bystander and the subject should completely
relax the arm. Following the measurement the subject will continue the protocol
as outlined below.
Study Timetable:
| TIME |
RPM |
FORCE |
| 0-3 min |
80 |
300 |
| 3-4 min |
MEASURE |
MEASURE |
| 4-7 min |
80 |
600 |
| 7-8 min |
MEASURE |
MEASURE |
| 8-11 min |
80 |
900 |
| 11-12 min |
MEASURE |
MEASURE |
| 12-15 min |
80 |
1200 |
| 15-16 min |
MEASURE |
MEASURE |
| 16-17 min |
RECOVERY |
RECOVERY |
| 17-18 min |
MEASURE |
MEASURE |
During testing the following parameters should be received in the table below:
Systolic Blood Pressure (SBP): The maximum pressure in the system
Diastolic Blood Pressure (DBP): The minimum pressure in the system
Mean Arterial Pressure (MAP): Time weighted average
of the SBP and DBP
Heart Rate (HR): The number of heart beats per minute
Perceived Exertion (PE): The subject's perceived work on a scale 1-10
Data Table:
| STAGE |
RPM |
FORCE |
PE |
SBP |
MAP |
DBP |
HR |
| 1 |
80 |
300 |
|
|
|
|
|
| 2 |
80 |
300 |
|
|
|
|
|
| 3 |
80 |
300 |
|
|
|
|
|
| 4 |
80 |
300 |
|
|
|
|
|
| 5 |
RECOVERY |
RECOVERY |
|
|
|
|
|
- Following testing, the data can be transferred from the
chart to a graph.
- SBP, DBP, MAP, HR, PE and work should be plotted versus
time.
LAB 4: Research Experiment
Suggested Time: 50 Minutes
Purpose:
To study a physical phenomenon such as the influence of
gender or age on the blood pressure in order to understand data acquisition,
analysis, and presentation.
Materials:
- computer
- DynaPulse hardware and software
Background:
Currently a great deal of medical research is focusing
on factors that may effect the blood pressure. Genetics, disease, and
aging process are only a few of the factors that may influence blood pressure
changes. Therefore, it is critical that we develop a method to systematically
evaluate observations.
Procedure:
Part A - Control Group Determination
1. In order to properly evaluate a phenomenon it is necessary to define
a control group. Determining control groups may be based on personal interpretation.
In most cases, the natural or common state is defined as the "control".
When studying the influence of age on blood pressure, a young group would
be selected as the control group due to the fact that a higher percentage
of young individuals have normal blood pressures. However, in studying the
influence of gender on blood pressure, males or females may be arbitrarily
selected as the control group.
Part B - Data Acquisition
1. In order to study the influence of gender on blood pressure, separate
the study group into males and females. In order to study the effects of
age, separate the study group into a young and old group. It should be noted
that the larger the study groups the more statistically significant the
results.
2. Designate a new group on the Student/Group directory and have each student
of the female/male or young/old group complete a seated and rested blood
3. Designate a new group on the Student/Group directory and repeat step
2 for the other group. Once again, make sure to save all measurements.
Part C - Data Analysis and Presentation
1. In order to statistically analyze and graphically display the results
for each group, use the Edit feature to “mask” any bad measurements
that may be the result of measurement artifact and should not affect the
study results.
2. The minimum, maximum, mean, and standard deviation for the systolic,
diastolic, mean arterial pressure, and heart rate can be calculated using
the Analysis feature. The normal distribution curves will be plotted for
each parameter as well.
3. The final results for each group should be presented as the mean +/-
the standard devia- tion for each parameter. For example the systolic blood
pressure may be presented as “127 +/- 4 mmHg”.
LAB 5: MEAN ARTERIAL PRESSURE DETERMINATION
Suggested Time: 30 minutes
Purpose:
To compare the DynaPulse mean arterial pressure measurement
with a simple approximation of the mean arterial pressure based on the
systolic and diastolic pressures.
Materials:
- computer
- DynaPulse hardware and software
Background:
The DynaPulse system is a clinical-grade blood pressure
device that actually measures the mean arterial pressure extremely accurately.
Traditional auscultatory blood pressure devices do not measure the mean
arterial pressure and therefore must approximate the value. A simple formula
was developed in which:
MAP = 1/3 SBP + 2/3 DBP
However, the formula above is only an approximation.
Procedure:
1. Select a group of individuals in which to compare the
mean arterial pressure measurement with the simple approximation.
2. Each member should complete a seated and rested blood pressure measurement
with the DynaPulse system. Make sure to save each measurement.
3. Complete the table below to compare the two techniques.
| STAGE |
SBP |
DBP |
MAP APPROX |
MAP MEASURED |
DIFFERENCE |
%DIFFERENCE |
| |
|
|
|
|
|
|
DIFFERENCE = MAPMEASURED - MAPAPPROX
%DIFFERENCE = MAPMEASURED - MAPAPPROX/ MAPMEASURED
4. After completing the table, calculate the
average value for each column by dividing the total by the number of subjects.
References
1. Cardiovascular Disorders. Springhouse: Springhouse,
1984.
2. Cardiovascular Physiology. New York: Oxford University Press, 1990.
3. Sixth Report of the Joint National Committee on Detection, Evaluation,
and Treatment of High Blood Pressure. U.S. National Institute of Health,
National Heart, Lung, and Blood Institute (NIH Pub. No. 98-4080), November,
1997.
4. Fishmen, AP ed. Circulation of the Blood - Men and Ideas. Bethesda, MD:
American Physiological Society, 1982.
5. Guyton, AC. Textbook of Medical Physiology. 8th ed. Philadelphia: W.B.
Saunders, 1991.
6. Human Physiology - Foundation and Frontiers. St. Louis: Times Mirror/Moshy
College Publishing, 1990.
7. Physicians Reference I. Pulse Metric, Inc. 1992.